بیماریهای زنان زایمان و نازایی
وب لاگ رسمی دکتر رویا پورقربان جراح و منخصص زنان زایمان و نازایی بورد تخصصی از دانشگاه تهرانبیماریهای زنان زایمان و نازایی
وب لاگ رسمی دکتر رویا پورقربان جراح و منخصص زنان زایمان و نازایی بورد تخصصی از دانشگاه تهراناهداء تخمک
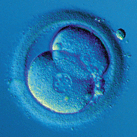
؛ اهداء تخمک؛
This proceeding is done to get a woman undergoing treatment pregnant using oocytes donated by another woman. With this technique, elderly women who have not succeeded in getting pregnant have a good chance of success
What is Oocyte Donation?
The Oocyte Donation Program offered by Plenitas is anonymous and voluntary, meaning that, unless otherwise agreed, recipients will not receive identifying information about the donor. In turn, the donor will not be given information about the identity of the recipient/s, neither will she know about the outcome of the oocyte fertilization, or if a pregnancy was achieved, or if a birth finally occurred. It is a voluntary act. The donor expresses her wish to donate, and gives her consent by signing a document containing the information received from different professionals in various consultations. The professionals provide donors with a detailed explanation of the steps to be taken to participate in the program, and the risks associated with donation. These steps include the preliminary examinations (medical, psychological, genetic and infectological tests) the donor must undergo to participate in the program. These proceedings are carried out in compliance with the guidelines set forth by the American Society of Reproductive Medicine (ASRM).
In what cases is Oocyte Donation applied?
Women who have already entered menopause due to age-related causes or other reasons. Women with deficient production of oocytes. Women with prior unsuccessful in vitro fertilization attempts. Women who are potential transmitters of hereditary diseases who wish to avoid transmitting them to their children.
Oocyte Donors: Requirements and Methodology
Volunteers willing to participate as donors should be aged 21 to 29. Donors are evaluated by a group of physicians and psychologists belonging to the institution in charge of the Oocyte Donation Program. The evaluation covers: a detailed questionnaire about history of genetically transmitted diseases of the patient and of her first and second degree relatives, blood karyotype, detection of the most frequent mutation of the cystic fibrosis disease, infectological tests to rule out HIV (AIDS), syphilis, hepatitis B, hepatitis C, and routine tests for a clinical evaluation, blood group, gynecological exam (with pap smear) and transvaginal ultrasound. If the prospective donor meets the requirements to join the program, she must express her willingness to do so by signing a document giving her consent. With this, the information process concludes, and she is recorded in an institutional registry where her clinical history, identity information, picture, physical traits, and psychological evaluation are filed. To be able to donate oocytes, the donor receives a medication (similar to that received by patients under assisted reproduction treatments) that stimulates ovulation and makes ovaries produce a larger number of eggs during that cycle. Then, when the donor's follicles have the appropriate size for ultrasound scan, the transvaginal ultrasound-guided aspiration is performed.
How is oocyte donation carried out and who can receive it?
This program offers the possibility to achieve pregnancy through the transfer of embryos obtained from the union of the donor's oocytes with sperm obtained from the husband, partner, or semen bank as the case may be. The technique used in Plenitas program to achieve egg fertilization is called ICSI, and it involves the microinjection of a single sperm into an egg. This technique seeks to evaluate the maturity of the eggs to offer eggs which are apt for normal fertilization. In addition, the injection of sperms makes the first step of the fertilization process easier. Once formed, the embryos are transferred to the recipient's uterus the second or third day following the microinjection.
Requirements to join the program as a recipient:
To be admitted into the program, recipients should not be older than 50.
Preparing the endometrial lining:
Once admitted into the Oocyte Donation Program, the recipient may start taking the medication necessary for the embryo transfer when her doctor deems it appropriate. The medication involves the administration of estrogens to make the endometrial lining highly receptive to the embryos.
The medication used for preparing the uterus depends on the presence or absence of ovarian activity in the recipient. If the patient is not menopausal, her cycle may interfere with the preparation of the uterus, and a medication (Lupron) is administered to suppress ovarian activity while the proceeding lasts. If the patient is menopausal (she has not menstruated for more than a year) there is no ovarian activity and, thus, the only proceeding is the preparation of the endometrial lining (uterus lining where the embryos are implanted). After the donor's follicle aspiration, at least four mature oocytes are set aside (Metaphase II). Afterwards, on that same day the oocytes are injected, and on the following day the fertilization is observed. The embryos are transferred within 48 or 72 hrs. after the aspiration. The program has a strict policy limiting to two the number of embryos to be transferred to the recipient in each attempt. This decision seeks to diminish the incidence of multiple pregnancy - which is an undesired outcome in an assisted fertilization proceeding.Applying this policy, the program's rate of global clinical pregnancy is close to 50%, based on statistics of 2004 and 2005, with a triple pregnancy incidence of 0%. Embryo transfer is a simple proceeding involving no risks, the resulting discomfort is similar to that of a pap smear, and it lasts 15 minutes approx. Once the transfer has been completed, the patient must rest for 48hrs. Two days prior to the transfer, Micronized Progesterone is administered to the patient, and its administration continues up to the third month of pregnancy.